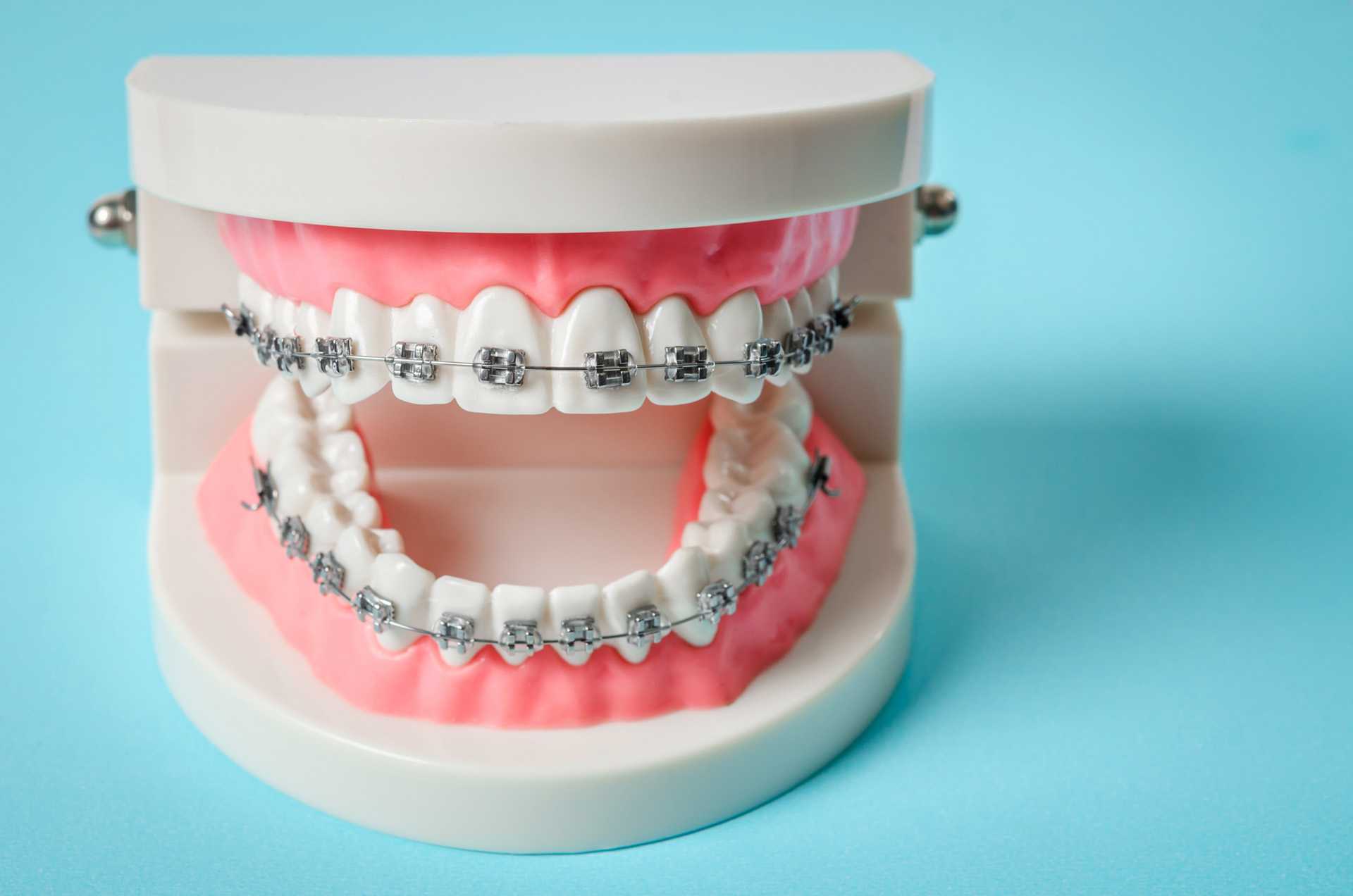
If you are researching how to qualify for Medicaid braces, the sections below outline the essentials and answer common questions such as, does Medicaid cover orthodontics and whether any states have programs that may have Medicaid cover braces for adults in limited circumstances.







Save $250 off braces or Invisalign!*
Schedule your appointment online.
Medicaid can make medically necessary orthodontic care affordable for children and adolescents. Not every child will qualify, but understanding your state’s rules and preparing a thorough application can improve the likelihood of approval. This guide explains how Medicaid approaches orthodontics, who may be eligible, how to apply, what benefits typically include, and how to get help if you receive a denial. If you are researching how to qualify for Medicaid braces, the sections below outline the essentials and answer common questions such as, does Medicaid cover orthodontics and whether any states have programs that may have Medicaid cover braces for adults in limited circumstances.
How Medicaid Covers Orthodontic Treatment
Medicaid is a joint federal–state program that provides health coverage to eligible low-income residents, including children, pregnant people, adults with disabilities, and older adults. Because states administer their own programs within federal guidelines, eligibility rules and covered services vary by state. Families often ask, does Medicaid cover orthodontics? The short answer is that it can for children when treatment is medically necessary, and coverage for adults is far more limited.
For children enrolled in Medicaid and the Children’s Health Insurance Program (CHIP), dental benefits are required under the Early and Periodic Screening, Diagnostic, and Treatment (EPSDT) benefit. EPSDT mandates coverage of services deemed medically necessary to correct or improve health conditions. This can include orthodontic treatment when a child has significant dental or skeletal issues that affect function. For adults, dental and orthodontic benefits are optional and differ widely; in most states, adult orthodontic coverage exists only for severe medical indications, if at all. If you are wondering if Medicaid pays for orthodontics, the answer depends on medical necessity and state policy, and whether the patient is a child or adult.
Orthodontics can be vital for children’s health and development. Severe bite problems (malocclusions) may interfere with chewing, speech, oral hygiene, and jaw function, and can contribute to pain or increased risk of tooth decay and gum disease. When braces are prescribed to address these functional problems rather than cosmetic concerns, Medicaid may cover evaluation and treatment if state criteria for medical necessity are met. Understanding how to qualify for Medicaid braces starts with determining whether the condition impairs function and meets your state’s medical necessity criteria.
Who Qualifies for Medicaid Braces
Basic Medicaid eligibility is determined by factors such as income, household size, age, disability status, and residency. Children and teens usually qualify through Medicaid or CHIP when household income meets state thresholds. Some states have expanded Medicaid for adults, but adult orthodontic coverage remains limited and is generally reserved for severe conditions requiring medical intervention. Whether any programs have Medicaid cover braces for adults depends entirely on state rules and is typically limited to complex medical needs.
To qualify specifically for braces under Medicaid, applicants must meet state-defined medical necessity standards. States often use screening tools or indices, such as a handicapping malocclusion index, to score the severity of bite problems. Conditions that may qualify include:
- Excessive overjet or underbite that causes difficulty chewing, speech issues, or lip incompetence
- Crossbites associated with soft tissue damage or abnormal wear
- Impacted teeth that cannot erupt without orthodontic intervention
- Cleft lip or palate and related craniofacial anomalies
- Skeletal discrepancies that impair function, such as chewing or speech
- Other documented problems that affect oral function or health
Mild crowding, minor spacing, and purely cosmetic alignment typically do not meet medical necessity standards. Age is also important; most coverage focuses on children and adolescents, and states frequently require that treatment begins before a specific age (often by age 18 or 21). Income eligibility follows your state’s Medicaid or CHIP rules. Because details vary, review your state Medicaid agency’s criteria or contact your managed care plan for exact standards and age limits. If you are evaluating does Medicaid cover orthodontics in your location, your state’s handbook or plan documents should outline medical necessity definitions and age cutoffs.
How to Apply for Medicaid Orthodontic Coverage
First confirm that you or your child is actively enrolled in Medicaid or CHIP. If you are not yet enrolled, apply through your state’s Medicaid portal or start at HealthCare.gov to be directed to the correct site. Once coverage is in place, follow these steps to pursue orthodontic benefits and ensure you understand how to qualify for Medicaid braces in your state:
- Schedule an evaluation with a provider who accepts your Medicaid plan. Many states require a referral from a general dentist to an orthodontist.
- Obtain complete diagnostic records. These usually include a comprehensive exam, facial and intraoral photographs, panoramic and cephalometric X-rays, and dental impressions or digital scans.
- Complete the prior authorization packet. Your orthodontist typically prepares and submits required forms, clinical notes, score sheets or indices, and supporting documentation to the Medicaid plan.
- Respond promptly to plan requests. If the plan asks for more information, provide it quickly to avoid delays.
- Await the decision. Approval letters specify covered services and timelines; denials include reasons and instructions for appeal.
You may be asked to provide proof of Medicaid eligibility, identification for the patient and parent or guardian, referral forms (if required), diagnostic records, a proposed treatment plan, and medical documentation from physicians or speech therapists that supports functional impairment. Clear documentation is essential when a plan reviews whether it will approve and pay; families often ask if Medicaid pays for orthodontics, and the outcome hinges on complete records that demonstrate medical necessity.
Common pitfalls that delay or jeopardize approvals include submitting incomplete records, using providers who are not in your Medicaid network, missing age cutoffs, and failing to keep contact information up to date. Retain copies of all submissions, attend scheduled evaluations, and notify your orthodontist and plan promptly if you move or switch managed care plans to prevent gaps in authorization.
What Medicaid Typically Covers for Braces
When orthodontic treatment is approved as medically necessary, Medicaid may cover a broad set of services. The specifics differ by state and plan, but commonly covered items include:
- Initial records and diagnostic workups
- Placement of braces or medically necessary appliances
- Periodic adjustments and monitoring visits
- Emergency visits related to orthodontic appliances
- Retention after treatment, such as retainers
For children, Medicaid often covers most or all authorized orthodontic fees when care is provided by in-network clinicians. Families may have little to no out-of-pocket cost for approved services. However, charges can occur for non-covered items, such as optional cosmetic enhancements, replacement of lost or broken appliances, or services performed outside the approved treatment plan. Review your authorization carefully and ask your orthodontist to explain any potential costs before treatment begins. If you are comparing whether Medicaid covers orthodontics and does Medicaid pay for orthodontics, remember that approval is based on medical necessity and network rules, not cosmetic preference.
The benefits go beyond finances. Correcting severe bite problems can improve chewing and speech, reduce abnormal tooth wear, make oral hygiene more effective, and lower the risk of cavities and gum disease. Addressing significant alignment issues early can also support healthy jaw development and may prevent more complex interventions later. Improved function often brings social and emotional benefits for children and teens.
Appealing a Denial and Getting Help
If your request is denied, read the denial letter closely to understand the reasons and the deadlines for appeal. Work with your orthodontist to submit a comprehensive appeal that directly addresses the plan’s concerns. Strong appeals often include updated measurements or photographs, functional assessments, additional letters from dentists, physicians, or speech therapists, and school or caregiver statements describing difficulties with chewing, speech, or oral hygiene.
Many states offer multiple levels of appeal, such as an internal plan appeal, a state fair hearing, and sometimes an external review. Each level has strict timelines. Keep copies of all correspondence and consider requesting assistance from your managed care plan’s member services, your state Medicaid agency, or a local health department. Dental schools and community health centers may have eligibility counselors who can help you navigate the process. These resources can clarify how to qualify for Medicaid braces under your state’s guidelines and whether any provisions exist that might have Medicaid cover braces for adults in exceptional medical cases.
Frequently Asked Questions
Do all children on Medicaid receive braces? No. Coverage is not automatic. Braces are approved when medical necessity criteria are met under state rules. Mild crowding or cosmetic concerns generally do not qualify.
Can adults receive Medicaid braces? Adult orthodontic coverage is uncommon and typically limited to severe medical needs, such as cleft palate care or pre-surgical orthodontics. Review your state’s adult dental benefits for details. Some states may have specific pathways where Medicaid covers braces for adults in very limited, medically complex scenarios.
How long does approval take? Prior authorization reviews often take several weeks. Timelines can be extended if records are incomplete or if the plan requests more information. Staying in close contact with your orthodontist’s office helps keep the review on track, especially when a plan determines whether it will approve and pay for care.
What if we change insurance plans or move? Notify your orthodontist and plan immediately. Transitions can interrupt authorizations, so coordinating early helps maintain continuity of care and coverage. This is especially important once treatment is approved, since gaps can affect whether the plan continues to pay.
Where can I find help or a participating provider? Contact your state Medicaid agency or your managed care plan’s member services. Dental schools and community health centers often provide counseling on benefits and eligibility. InsureKidsNow.gov can help you locate Medicaid and CHIP dental providers. Your orthodontist’s office is also a valuable resource for submitting authorizations and appeals.
Key Takeaways for Qualifying
- Coverage for braces under Medicaid depends on medical necessity, not cosmetic preference.
- Eligibility and criteria vary by state; confirm age limits, required referrals, and scoring tools used to assess severity.
- Use in-network providers, submit complete diagnostic records, and keep organized copies of everything.
- Start early to meet age requirements and allow time for prior authorization and possible appeals.
- If denied, appeal within deadlines and add detailed documentation of functional problems.
With the right information and thorough documentation, families can navigate Medicaid’s process more confidently and secure needed orthodontic care when it is medically necessary. If you are researching how to qualify for Medicaid braces and asking does Medicaid cover orthodontics or does Medicaid pay for orthodontics in your state, reach out to your plan and orthodontic provider for the most current, state-specific rules. Adults should carefully review whether any provisions exist that have Medicaid cover braces for adults in limited, medically necessary situations.